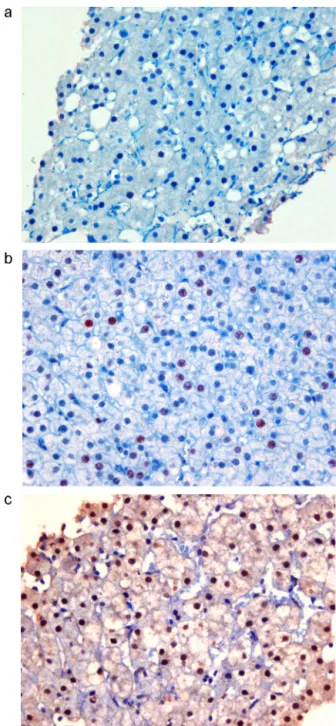
Lack of association of hepatic estrogen receptor-alpha expression with histopathological and biochemical findings in chronic hepatitis C
Tam metin
Şekil
Benzer Belgeler
Yani uygulama öncesi kontrol ve deney grubu öğrencilerinin fene yönelik motivasyonun altıncı ve son alt faktörü olan öğrenme ortamındaki özendiricilik
This study aimed to statistically establish the relationship between HBV-DNA level and hepatic histopathology in patients who were diagnosed with chronic hepatitis and planned
The Relationship between the Serum RNA Titers of Hepatitis C Virus and Biochemical Parameters in Chronic Hepatitis C Patients Viral Hepatitis J
Aim: To evaluate the prevalence of adenotonsillar Actinomyces with histopathological findings and to determine the relationship of Actinomyces with allergic rhinitis
Allele distribution in ERβ showed no significant difference between the normal allele G and mutant allele A in the case group compared with the control group, which means that
Given that there are problems concerning the representation, election, and functioning of those councils, in addition to their negative image among students and
The power capacity of the hybrid diesel-solar PV microgrid will suffice the power demand of Tablas Island until 2021only based on forecast data considering the
Pandya, S., Ghayvat, H., Shah, J., Joshi, N., A Novel Hybrid based Recommendation System based on Clustering and Association Mining, 10th IEEE International Conference on